Gut-Brain Axis & My Personal Story
Mar 31, 2022The Beginning (sort-of)
When I was 25 years old and working as a new nurse in the emergency department (on night shift no less), I began having digestive issues. It all began with your run-of-the-mill reflux. And like any good little patient, I consulted with my PCP. Bless him, he put me on reflux medication. Protonix, I believe. Or Prilosec. I can’t quite remember but you get the idea. It was standard of care. He also ordered a barium swallow study to prove that I was having reflux. The test came back positive. How many of you have gone through similar situations? Have a symptom? Here’s a pill! There was no consideration that I was extremely stressed at work and my circadian rhythms were a mess from working night shift. I was diagnosed with GERD and IBS.
Somewhere deep down, I knew there had to be a better way. I was also suffering with bloating and alternating diarrhea and constipation. TMI. I know! I changed jobs and switched to day shift. The reflux improved somewhat. I stopped taking my reflux medication but I was still having the other digestive issues.
After hours of surfing Google for answers, I discovered something called a Low-FODMAP diet. This lower fiber diet would allegedly heal my woes and lead to digestive bliss. It is an acronym that explains the different carbohydrates you’re eliminating. Sign me up! My husband, Paul, was horrified. I found this lovely RD who provided a printable handout and I dedicated a whole shelf in the pantry to me and my low-FODMAP foods. I went all in and eliminated a ton of foods, including onions and garlic. Onions and garlic. The two foods that go well with everything!

Here’s the thing, though: after 2-3 days, I felt amazing! No more bloating. No more pain. Regular poops, which if you know me now, you know that’s a high metric for health in my book.
I stayed on that diet without cheating for about 5 weeks. After that, I slowly added foods back in and I remember noticing an upper limit. If I had a few high-fiber foods, I was okay, but a ton of raw, high-fiber foods and I was back to being bloated and uncomfortable. For years, I simply modified my diet to suit my digestive system and it all worked really well until I discovered I had mold toxicity.
Mold Toxicity
Turns out, the home we were living in had black mold in an area where the roof was leaking. After the birth of our first child, Jack, I complained frequently about feeling exhausted. More than exhausted. Bone-deep weary and ready to turn into Rip Van Winkle at any moment. People kept reassuring me that this was normal and all postpartum fatigue. Again, my intuition kept telling me to dig deeper.
Remember that PCP who put me on the reflux medication? Well lo and behold, I ended up working with him after graduating as a nurse practitioner. And while I was busy healing myself with a self-imposed low-FODMAP diet, he was busy becoming certified as a Functional Medicine Practitioner. In his defense, he wouldn’t have put me on the Prilosec today! I signed up to work with him in the functional medicine practice. After about 3-4 months of labs and investigating, we finally discovered the markers for mold. Ultimately, we moved to a new home and I treated myself for mold. It worked so well that I “accidentally” got pregnant with our second child, Ellie Grace, and I was able to cruise through the postpartum period with more energy than ever before. I must have been feeling so good that I forgot to use the diaphragm I’d asked my midwife to prescribe because at nine months postpartum, I got pregnant again! Sheesh.

Living the "Rare" Life
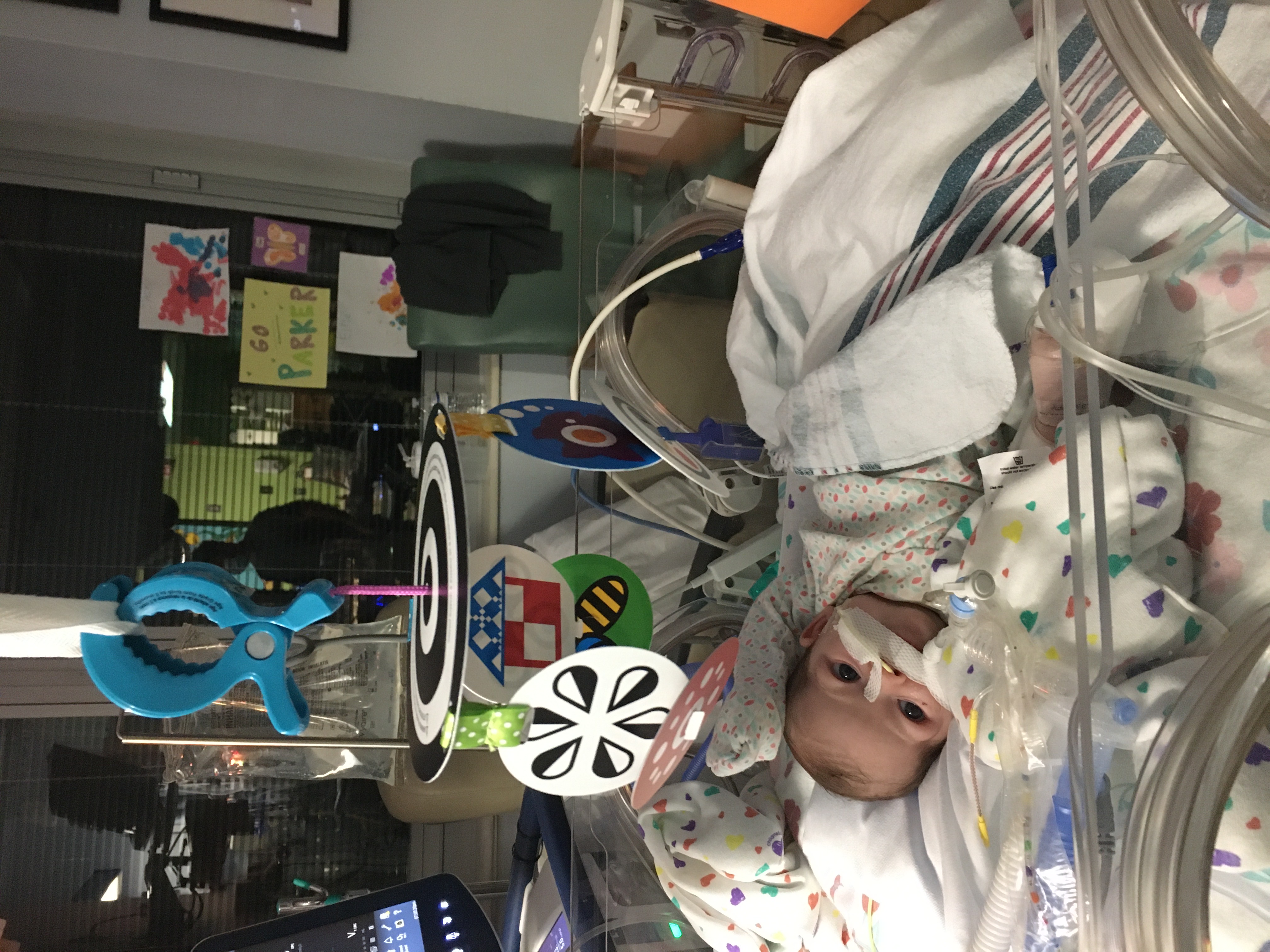
Everything seemed to be going so well. I had another uncomplicated pregnancy and a third natural, unmedicated childbirth to welcome our sweet Parker into the world. She was lovely, but on her 10th day of life, something seemed off. We were shooting newborn and family photographs that day and we kept noticing she had a runny nose and was looking sort of pink when she fell asleep. Her color was off. During a lactation appointment that afternoon, she wouldn’t wake up to nurse. We peeled off her clothes to discover that she was retracting and had nasal flaring. To those who don’t know, this means the child is in respiratory distress and it’s an emergency situation.

We ultimately ended up in the ER where Parker was poked and prodded and admitted to the PICU. A few hours later, she was diagnosed with rhinovirus, the common cold. She needed deep suctioning and some assistance with oxygen through a nasal cannula (that tube thing that goes under your nose). Straightforward, right? We thought so too. But a few days later, we went to wake her up and she was floppy, pale, and unresponsive. They rushed her to the PICU - we had been downgraded to the regular pediatric floor a few days prior. Looking back, that was the worst hour of my entire life. I was convinced that she was going to die. It’s even hard to type. Anyone who has ever suffered through trauma gets me right now.
They intubated her and treated her for the pneumonia secondary to her cold… and then things got weird. They said she wasn’t trying to breathe on her own over the ventilator. The physician suggested it was an apnea she’d outgrow or something more complicated, a rare genetic disorder. He suggested we be transferred 15 minutes away to Virginia Commonwealth University, the local teaching hospital in Richmond, Virginia.
I’ll spare the details and the agonizing hours spent on hospital benches, pumping with residents and nurses all around me, sleeping in a hospitality house, and binge watching Netflix with her beside me in any attempt to escape my reality. Those were some dark days. Paul and I clung to each other both physically and emotionally. And then on Friday the 13th, November 2020, we were told that our sweet little baby girl does in fact have congenital central hypoventilation syndrome (CCHS). That afternoon, I’ll never forget the looks we got from the physicians, nurses, and case workers in our meeting to discuss the plan. They couldn’t help it but they looked at us with this pity that still makes me feel queasy. It was like we were tossed into the deep end of the pool with no life raft and only a basic understanding of how to swim.
In some ways, it was a relief to have a diagnosis and plan of attack. Parker doesn’t breathe effectively when she sleeps and requires ventilation to sleep. She had a tracheotomy procedure a week later and we began the grueling process of becoming special needs parents. This involved finding nurses, managing equipment, learning how to care for her, and being trained on the machines. When she’s older, she’ll have three different options for ventilation: mask, trach, or implanted pacers. For now, she has a trach. We’ve grown so much in the almost year and a half she’s been alive.
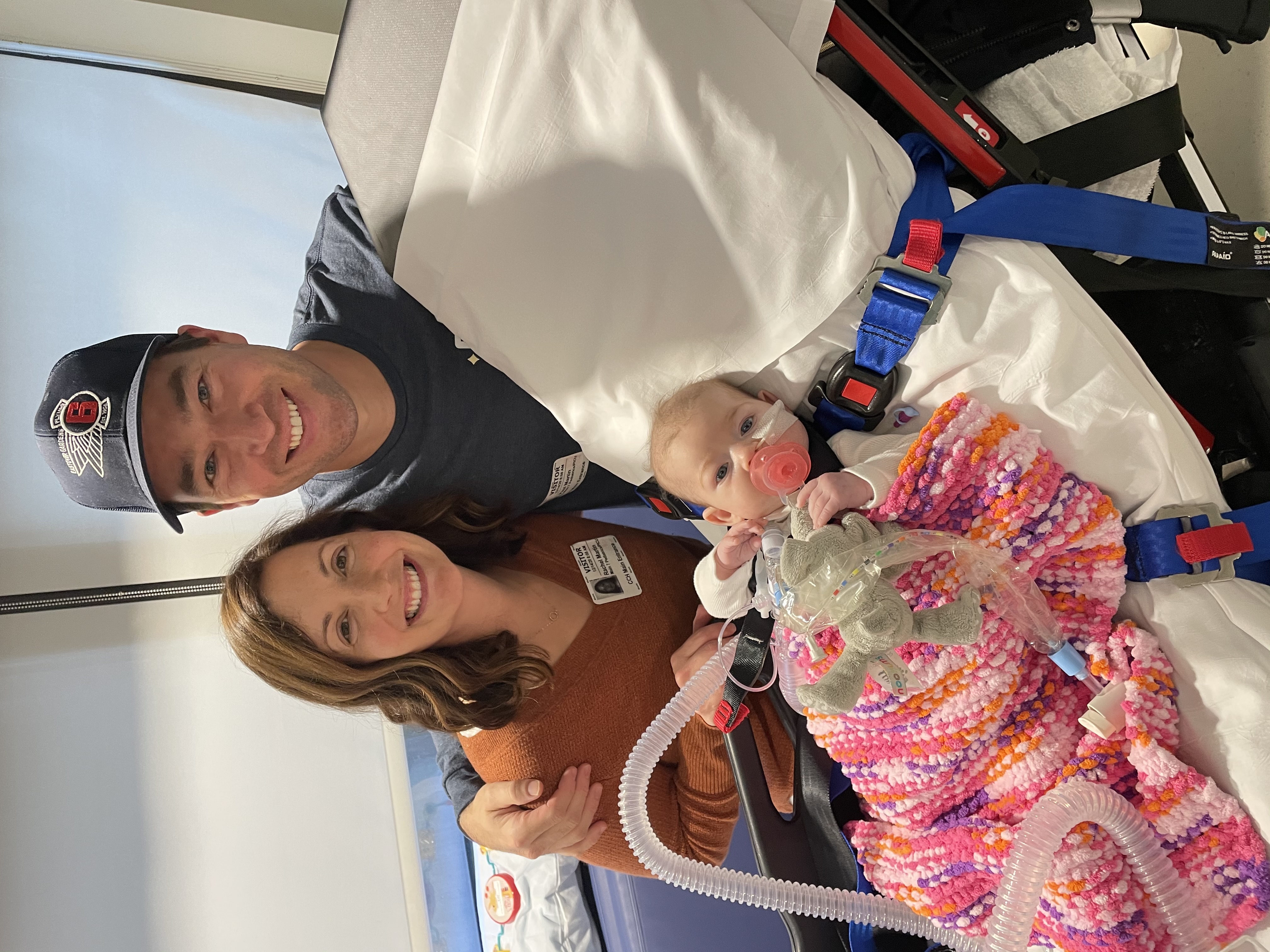
Being discharged home after almost 2 months!
Regardless, chronic stress in the form a kiddo with a rare disease plus sleep deprivation is part of our daily lives. Nursing is very difficult to come by these days, so we take turns “being in charge” and answering alarms. Paul’s job as a firefighter working 24 hour shifts makes it all even more difficult. Sleeping through the night is a luxury to me now that I’m rarely afforded. So what’s a girl to do?

Vagus Nerve
I leverage what I can and I always bring it back to the gut-brain relationship. We have this nerve, the vagus nerve, that runs down from our brains all the way to our guts. It’s part of the parasympathetic nervous system, or what most people know of as the “rest and digest” system. That is my main focus. What can I do to stimulate that? For me personally, I feel the best when I do these things:
- Therapy - I’m putting this one first because it was the most important thing for me
- Eat an anti-inflammatory diet of lower carbs, moderate fats, moderate protein
- Eat at least 5 servings of veggies daily and at least 1 serving of fermented food
- Avoid processed foods and sugar
- Lots of filtered water
- Avoid caffeine and alcohol - I only drink green tea
- Sunshine
- Easy exercise - Yoga, barre, and walking
- Go to bed early!
- Journal, meditation - Working on being more consistent with these
- Acupuncture
- Dry brushing, sauna blanket
- Supplements

To summarize, I’ve endured digestive issues, inflammatory mold that lead to more digestive issues, and chronic stress. I know what it’s like to not be able to change a situation but instead figure out how to endure it. In many ways, I feel like I’m stronger because of it. I wouldn’t change a thing. Parker has given more to us than we’ve given to her. I’m brave, compassionate, faithful, and I live in the moment now. Life is short, right? I feel this simultaneous pull to prioritize my health so I can enjoy my life but not dwell on it or get wrapped up in what I can’t control. I don’t want to miss the whole point. I change what I can and leave the rest. And that’s what I’m inspiring others to do too.
How can you leverage what’s in our control to positively impact your health? And if you need some help figuring all of this out, I’m happy to help!
Remember: this post is for informational purposes only and may not be the best fit for you and your personal situation. It shall not be construed as medical advice. The information and education provided here is not intended or implied to supplement or replace professional medical treatment, advice, and/or diagnosis. Always check with your own physician or medical professional before trying or implementing any information read here.